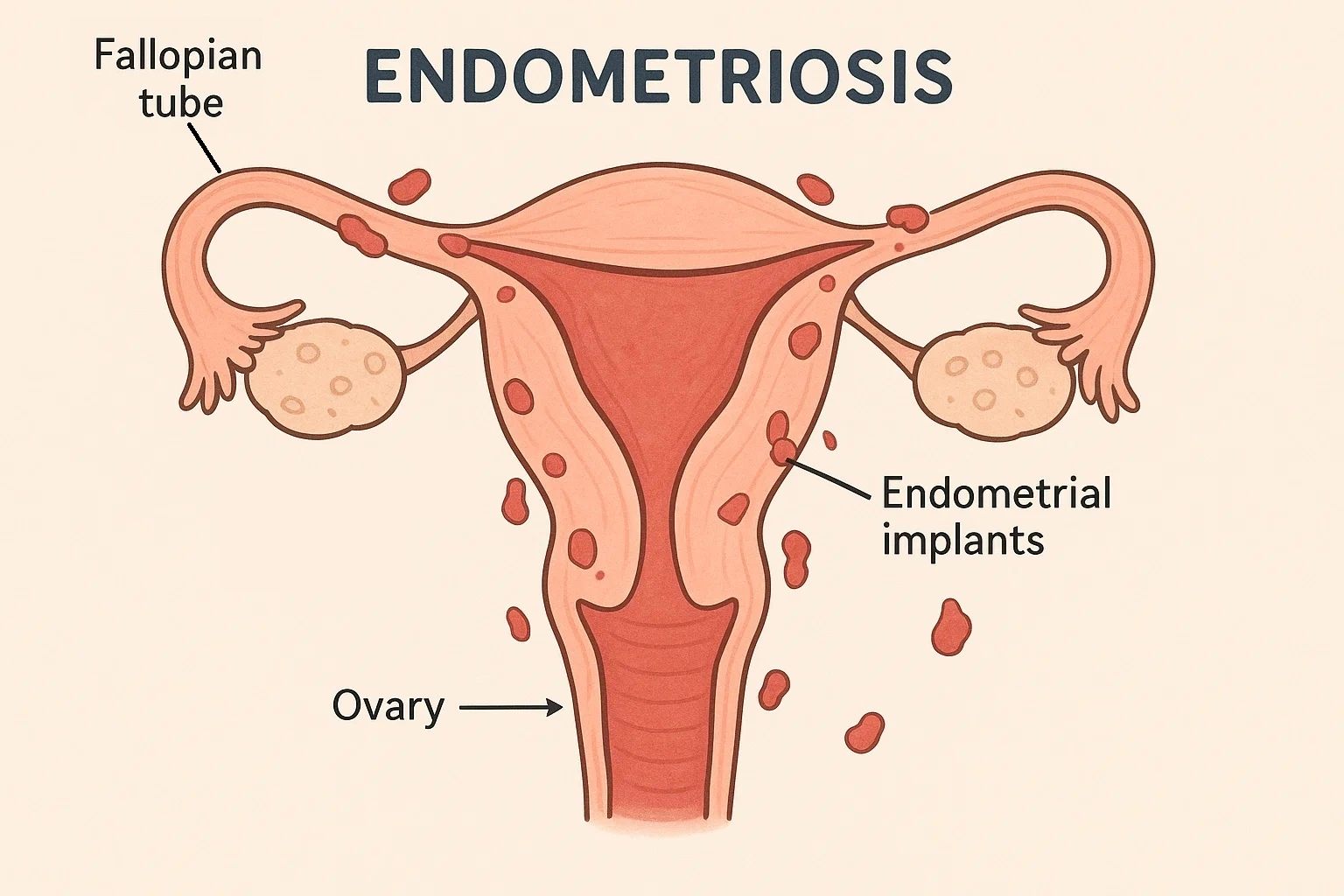
Female Reproductive Hormones and Their Functions: How Hormones Affect Fertility
For women trying to conceive, hormones can feel overwhelming. Terms like FSH, LH, AMH, and progesterone show up in test results and clinic consultations, but what they actually do is rarely explained in easy language.
Understanding female reproductive hormones and their functions helps women recognize what is happening in their body, spot early warning signs, and have better conversations with their consultant. This article breaks it all down simply.
What Are Female Reproductive Hormones?
Female reproductive hormones are chemical messengers produced by the brain, pituitary gland, and ovaries. They control the menstrual cycle, trigger ovulation, prepare the uterus for implantation, and support early pregnancy. Each hormone has a specific job, and they work in a timed sequence. When one falls out of balance, the entire cycle can be affected.
The role of hormones in female fertility goes beyond just ovulation. They also govern egg quality, uterine receptivity, and cervical mucus production. A single hormonal imbalance can disrupt multiple stages of the conception process at once.
Key Female Reproductive Hormones and Their Functions
Estrogen:
The main female sex hormone. Estrogen and fertility are closely linked. It drives follicle growth, thickens the uterine lining, and improves cervical mucus to help sperm move. Estrogen peaks just before ovulation and triggers the LH surge that releases the egg.
Progesterone:
The body produces progesterone after ovulation. Progesterone and fertility are inseparable. It stabilizes the uterine lining and creates the right conditions for implantation. Low progesterone after ovulation is a common reason for failed implantation and early pregnancy loss.
FSH (Follicle Stimulating Hormone):
FSH and female fertility are directly connected. The pituitary gland releases FSH to stimulate the ovaries to grow follicles, each containing a potential egg. High FSH levels can signal reduced ovarian reserve, meaning the ovaries need extra stimulation to produce a mature egg.
LH (Luteinising Hormone):
LH hormone and ovulation are directly linked. A sudden LH surge triggers the ovary to release a mature egg. Ovulation predictor kits work by detecting this LH surge to identify the fertile window.
AMH (Anti-Mullerian Hormone):
AMH hormone levels show how many eggs a woman has left, known as ovarian reserve. AMH stays relatively stable throughout the cycle and can be tested at any time. Low AMH means fewer eggs are available, which affects both natural conception and IVF planning.
Prolactin:
Prolactin controls milk production after childbirth. But high prolactin levels outside of breastfeeding can suppress ovulation and cause irregular or absent periods. Prolactin and infertility are connected through this hormonal suppression.
Thyroid Hormones:
The thyroid and female fertility are more closely connected than most people expect. Both an underactive thyroid (hypothyroidism) and an overactive thyroid (hyperthyroidism) can disrupt ovulation, cause irregular cycles, and raise the risk of miscarriage. Doctors routinely check thyroid function during fertility evaluations.
Insulin:
Insulin resistance, strongly linked to PCOS and hormonal imbalance, throws off the balance of reproductive hormones. High insulin levels push the ovaries to produce excess androgens, which block normal follicle development and prevent ovulation.
How These Hormones Work Together During a Fertility Cycle
Understanding how hormones affect ovulation means looking at the full cycle, not just individual hormones. Each phase follows a specific hormonal sequence, and normal hormone levels for conception must be present at each stage for the process to work.
In the follicular phase, FSH rises and drives follicle development. As follicles grow, estrogen increases and thickens the uterine lining. At mid-cycle, rising estrogen triggers an LH surge, which causes the ovary to release a mature egg. Then begins the luteal phase. The empty follicle becomes the corpus luteum, which produces progesterone to prepare the lining for implantation.
If implantation occurs, the embryo produces HCG, which signals the corpus luteum to keep making progesterone. If it does not, progesterone drops, the lining sheds, and a new cycle starts. A disruption at any point, whether from low FSH, weak estrogen response, a missed LH surge, or low progesterone, can stop conception from happening.
Hormonal Imbalance and Female Infertility
Hormonal imbalance and infertility are closely connected. The most common reasons for female hormone imbalance include PCOS and its associated hormonal imbalance, thyroid disorders, elevated prolactin, insulin resistance, age-related decline in ovarian reserve, and significant weight changes.
The early symptoms of hormonal imbalance affecting fertility are not always obvious. Common signs of hormonal imbalance in women include:
- Irregular, absent, or very painful periods
- Unexplained weight gain or difficulty losing weight
- Persistent acne, especially along the jawline
- Excessive hair growth on the face or body, or hair thinning on the scalp
- Mood swings, anxiety, or low energy without a clear cause
- Difficulty conceiving despite regular unprotected intercourse
- Recurrent early pregnancy loss
Each hormone must fall within a specific range at the right phase of the cycle for pregnancy to happen. A fertility hormone blood test covering FSH, LH, oestradiol, AMH, prolactin, progesterone, and thyroid hormones gives a clear picture of where imbalances exist.
Lifestyle Factors That Influence Hormonal Balance
The impact of lifestyle on hormonal balance is significant and often underestimated. These everyday habits directly affect fertility hormone levels in females:
- Sleep: Poor sleep raises cortisol and lowers melatonin, both of which interfere with reproductive hormone regulation.
- Stress: Chronic stress keeps cortisol high, which suppresses GnRH, the hormone that tells the pituitary to release FSH and LH.
- Weight: Being overweight or underweight both affect estrogen levels. Excess fat tissue produces extra estrogen, throwing off the hormonal feedback loop.
- Exercise: Too much high-intensity exercise can suppress ovulation. Moderate, regular activity supports insulin sensitivity and hormonal balance.
- Screen time and light exposure: Late night screen use suppresses melatonin, which plays a role in the reproductive hormonal cycle.
- Diet: High sugar intake and processed foods worsen insulin resistance, particularly for women with PCOS and hormonal imbalance.
Natural Ways to Support Hormone Balance
For women exploring how to balance female fertility hormones naturally, these evidence-supported steps can make a real difference:
- Diet and micronutrients: Foods that balance female hormones include leafy greens, lentils, flaxseeds, pumpkin seeds, walnuts, moringa, and whole grains. These supply zinc, magnesium, B vitamins, and omega-3 fatty acids that support hormone production.
- Gut health: The gut plays a role in estrogen metabolism. Fibre-rich foods and fermented foods like curd support a healthy gut and help maintain normal estrogen levels.
- Cycle tracking: Tracking basal body temperature and changes in cervical mucus helps identify ovulation patterns and can flag hormonal irregularities early.
- Stress reduction: Consistent stress management through light exercise, breath work, and better sleep lowers cortisol and supports the hormonal environment needed for conception.
- Limiting toxins: Reducing exposure to endocrine-disrupting chemicals in certain plastics, pesticides, and personal care products supports long-term hormonal balance.
When to Seek Medical Help
Natural support is valuable, but hormonal imbalance treatment for fertility sometimes requires medical intervention. Hormonal causes of infertility are among the most common and most treatable, which makes early testing worthwhile. A proper evaluation is recommended in the following situations:
- Periods are consistently irregular, absent, or unusually painful
- Symptoms of hormonal imbalance such as unexplained weight gain, hair loss, or persistent acne are present
- Trying to conceive for 12 months without success, or 6 months if over 35
- A known diagnosis of PCOS, thyroid disorder, or elevated prolactin
- Recurrent miscarriage or failed implantation
A female hormone test for fertility typically starts with a day 2 or day 3 blood test measuring FSH, LH, oestradiol, and prolactin, along with AMH and thyroid hormones. Doctors use these results to determine whether treatment involves medication, lifestyle changes, or assisted reproductive procedures. Learning how to increase fertility hormones naturally through diet and lifestyle is a useful first step, but medical testing provides the full picture.
Conclusion
Female reproductive hormones and their functions work together in a precise sequence to make conception possible. Estrogen, progesterone, FSH, LH, AMH, prolactin, thyroid hormones, and insulin each play a distinct role. An imbalance in any one of them can affect fertility at multiple stages.
Most hormonal causes of infertility are identifiable through the right tests and treatable with the right plan. Lifestyle changes help, but when symptoms persist or conception is delayed, a proper medical evaluation gives couples the clarity they need to move forward.
At Sudha Fertility Centre, Dr. S. Dhanabagyam and Dr. S. Pradeepa focus on precise diagnosis before treatment, ensuring every recommendation is based on the specific cause rather than a general approach. If hormonal imbalance is affecting fertility, the right evaluation is the first and most important step.

Dr. S. Pradeepa is a fertility specialist at Sudha Fertility Centre, Erode, with expertise in IVF, IUI, ICSI, PCOS, and endometriosis. She holds MBBS, DGO, DNB (OG), and a Fellowship in Reproductive Medicine. Known for her patient-centric approach, she provides personalized, evidence-based care and reviews medical content to guide informed fertility decisions.