
The Unconventional Guide: How Folic Acid Helps in Pregnancies
How Folic Acid Helps in Pregnancies
- What happens if you don’t take folic acid during pregnancy? Risks of neural tube defects including Spina Bifida and Anencephaly
- Folic acid tablets for pregnancy Folic acid as the synthetic form of Vitamin B9 and its role in neural tube and red blood cell development
- When to stop taking folic acid in pregnancy Supplementation is generally recommended up to 12 weeks, though continuing is safe
- Folic acid dose for pregnancy women Age-based daily intake breakdown with higher amounts for pregnancy and breastfeeding
- Folic acid supplementation in early second trimester Post-12-week supplementation may support the child’s cognitive development
- Folic acid supplementation in early second trimester Post-12-week supplementation may support the child’s cognitive development
- How long after taking folic acid will I get pregnant? Start 2–3 months before conception; diet alone is not sufficient, supplementation is necessary
One of the most essential nutrients for pregnancy is folic acid. The benefits of folic acid are vast, and loads of research have shown that when this nutrient is started in the months preceding pregnancy, it has important health benefits for expecting women and their babies. Folic acid aids the proper closure of the embryonic neural tube, which is the precursor to your baby’s brain and spinal cord, during the first few weeks of pregnancy. It also aids in the development of your baby’s heart and circulatory system, as well as lowering the risk of some birth defects. Here, at Sudha Fertility Centre, we provide you with highly qualified Gynecologists who will guide you throughout your journey of becoming a mother.
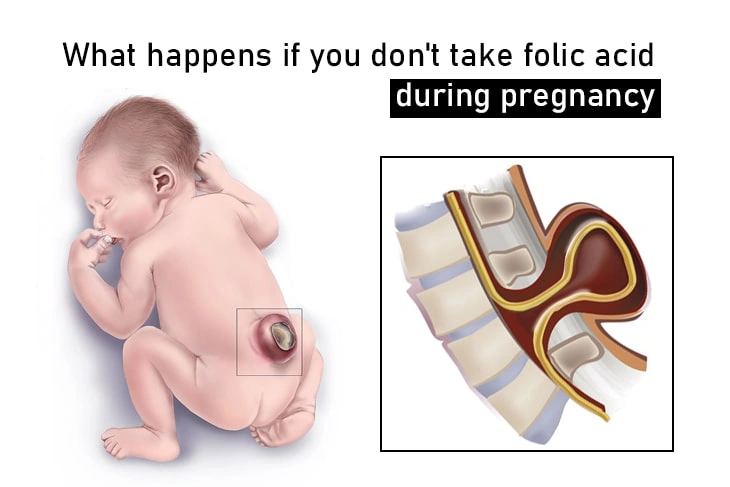
What happens if you don’t take folic acid during pregnancy?
Your baby is more likely to have neural tube defects if you don’t get enough folic acid before and after birth. Neural tube defects are life-threatening birth defects that affect the spine, spinal cord, or brain. These include:
- Spina bifida: This disorder occurs when the spinal column of an unborn baby does not completely close during growth in the womb, exposing the spinal cord. As a result, the muscles controlling the legs and other organs are paralyzed. Spina bifida affects children for the rest of their lives. They can also need a number of surgeries.
- Anencephaly: This means that most or all of the brain and skull does not develop in the womb. Almost all babies with this condition die before or soon after birth.
Folic acid tablets for pregnancy
Folic acid is a synthetic version of the B vitamin folate. Folate aids in the formation of red blood cells and the development of your baby’s neural tube into their brain and spinal cord.
Every day, 400 micrograms of folate are recommended for all women of childbearing age. Check to see if your multivitamin contains the recommended amount of vitamins if you take it every day. You can take folic acid tablets instead of a multivitamin if you don’t want to take one.
When to stop taking folic acid in pregnancy
Your baby’s spine will have grown by the time you reach 12 weeks pregnant, so you can avoid taking folic acid. You can, however, continue to take supplements after 12 weeks if you wish, and it will not affect your infant. Folic acid, as well as other important vitamins for a healthy pregnancy, such as vitamin D, can be found in pregnancy vitamins and supplements that are designed to be taken all the way through pregnancy.

Folic acid dose for pregnancy women
The prescribed dietary allowance (RDA) requires the folate you get from both food you consume and any supplements you take.
0-6 months: 65 micrograms/day adequate intake (AI)
7-12 months: 80 micrograms/day adequate intake (AI)
1-3 years: 150 micrograms/day adequate intake (AI)
4-8 years: 200 micrograms/day adequate intake (AI)
9-13 years: 300 micrograms/day adequate intake (AI)
14 years and above: 400 micrograms/day adequate intake (AI)
Pregnant women: 600 micrograms/day adequate intake (AI)
Breastfeeding women: 500 micrograms/day adequate intake (AI)
Gynecologists recommend that all pregnant women take at least 600 micrograms (mcg) of folic acid daily. This level of folic acid is found in most prenatal vitamins.
It is possible that taking folic acid after you find out you’re pregnant isn’t enough. Many women don’t know they’re pregnant until they’ve been pregnant for 6 weeks or longer. Neural tube defects usually appear in the first month of pregnancy, before you even know you’re expecting.
The CDC recommends that women who plan to become pregnant or who are of childbearing age take 400 mcg of folic acid daily to ensure they have enough folic acid in their bodies to prevent neural tube defects.
If you’ve already given birth to a child with a neural tube defect, you might need higher doses of folic acid in the months leading up to your next pregnancy and during the first few months of pregnancy. Your doctor will help you determine the proper dosage.
Folic acid supplementation in early second trimester
The neural tube of the baby should have closed by 12 weeks, so you won’t need to take folic acid. But it isn’t harmful to take it all the way through your pregnancy. So, you can carry on if you are taking pregnancy multivitamin pills that contain it.
Folic acid supplementation after the early period recommended to prevent NTD can have a positive impact on the child’s cognitive growth. There is a need for more randomised trials in pregnancy and follow-up in childhood.
How long after taking folic acid will I get pregnant?
Ideally, you should take folic acid supplements for two to three months before you conceive and until you are 12 weeks pregnant. This helps it to build up in your body to the point that it protects your future baby from neural tube defects like spina bifida.
Knowing when to take folic acid and how much to take will help you launch your fertility journey on the right foot.
The Center for Disease Control (CDC) and Prevention recommends that women take 400 micrograms (mcg) of folic acid every day for one month before attempting to conceive.
You may also increase your intake of folate, which is the natural source of folic acid, by eating more foods that contain it. Even a balanced diet, however, does not provide enough folic acid for pregnancy, so taking folic acid supplements is necessary.

Take your folic acid-rich daily prenatal vitamin to keep up the good work on the nutrition front. This supplement, combined with a balanced diet, is an ideal way to start off your new baby’s life.
Frequently Asked Questions
How much folic acid should I take during pregnancy?
When should I start taking folic acid before pregnancy?
What happens if I don't take folic acid during pregnancy?
When should I stop taking folic acid during pregnancy?
What is the difference between folic acid and Folate?
Can I get enough folic acid from food alone?
What foods are rich in folic acid/folate?
Does folic acid help with fertility or getting pregnant?
Can folic acid reduce the risk of miscarriage?
What should I do if I've previously had a baby with a neural tube defect?

Dr. S. Pradeepa is a fertility specialist at Sudha Fertility Centre, Erode, with expertise in IVF, IUI, ICSI, PCOS, and endometriosis. She holds MBBS, DGO, DNB (OG), and a Fellowship in Reproductive Medicine. Known for her patient-centric approach, she provides personalized, evidence-based care and reviews medical content to guide informed fertility decisions.





Permalink
Permalink